Oral surgery is a specialized dental procedure that involves surgical intervention to treat conditions affecting your mouth, teeth, jaw, and surrounding tissues. Oral surgeons perform surgical procedures when traditional dentistry cannot adequately address the problem or when surgical intervention is the most effective treatment option.
In simple terms: Your oral surgeon uses specialized surgical techniques to treat complex conditions affecting your mouth and jaw that require surgical expertise.
Essential Facts About Oral Surgery
What it is: Surgical treatment for mouth, teeth, and jaw conditions performed by a trained oral maxillofacial surgeon
Why you might need it: Complex tooth extraction, dental implant placement, jaw misalignment, bone deficiency, or oral pathology treatment
Common procedures: Tooth extraction, dental implants, jaw surgery, bone grafting, oral pathology treatment
Procedure time: 30 minutes to 3 hours depending on complexity
Recovery: 1-2 weeks for routine procedures; 6-12 weeks for complex cases
Anesthesia: Local anesthesia, IV sedation, or general anesthesia
What is Oral Surgery
Oral surgery, also called oral and maxillofacial surgery, is a surgical specialty focusing on diagnosis and surgical treatment of diseases, injuries, and defects affecting the mouth, teeth, jaws, and surrounding tissues. Oral surgeons receive extensive training beyond dental school, completing four additional years of surgical residency to develop expertise in complex surgical techniques.
The field combines dentistry with surgical principles, requiring specialized knowledge of facial anatomy and surgical intervention. Oral surgeons work in hospitals, surgical centers, and private practices, managing both routine cases and complex reconstructive procedures. At Talpadent, our experienced oral surgeons provide comprehensive surgical solutions for a full range of dental and maxillofacial conditions, from routine extractions to complex reconstructive cases.
Types of Oral Surgery Procedures
Oral surgeons perform the following major types of surgical procedures:
- Tooth Extraction – Surgical removal of teeth that cannot be saved or must be extracted
- Dental Implants – Surgical placement of artificial tooth roots to support replacement teeth
- Jaw Surgery (Orthognathic Surgery) – Surgical correction of jaw alignment problems
- Bone Grafting – Surgical restoration of missing jawbone tissue
- Oral Pathology Treatment – Surgical removal and treatment of abnormal tissue conditions
- TMJ Disorder Treatment – Surgical intervention for temporomandibular joint problems
Tooth Extraction
Tooth extraction is the most common oral surgery procedure. While general dentists extract many teeth, oral surgeons handle complicated cases. If you’re dealing with wisdom teeth issues, our dedicated wisdom teeth removal guide covers when extraction is necessary and what to expect.
Surgical extractions required when:
- Teeth are impacted (trapped beneath bone or gum tissue)
- Teeth have curved or broken roots
- Teeth are severely decayed and crumble during extraction
- Wisdom teeth require bone removal for safe removal
Surgical advantages:
- Precise removal using specialized techniques
- Better outcomes for difficult extractions
- Reduced trauma to surrounding tissues
- IV sedation or general anesthesia available
Dental Implants
Dental implants are artificial tooth roots surgically placed into the jawbone to support replacement teeth. Explore our complete guide to dental implants to understand the entire process from evaluation to final restoration.
Why implants are chosen:
- Preserve jawbone (unlike dentures which cause bone loss)
- Function like natural teeth with strong bite force
- Appear identical to natural teeth
- Last 20+ years with proper care
Surgical requirements:
- Adequate jawbone volume (bone grafting needed if insufficient)
- 3D imaging and surgical planning for precise placement
- 3-6 months for bone integration with implant
- Crown placement after healing
Jaw Surgery (Orthognathic Surgery)
Orthognathic surgery corrects jaw alignment problems affecting function, appearance, or breathing. Our orthognathic surgery guide explains how jaw surgery combined with braces addresses severe bite problems.
Problems addressed:
- Severe overbite or underbite
- Open bite (front teeth don’t touch)
- Severe facial asymmetry
- Sleep apnea from airway obstruction
- Difficulty chewing or swallowing
Procedure benefits:
- Restores proper function (chewing, swallowing, breathing)
- Creates balanced facial appearance
- Improves sleep quality
- Significant confidence boost

Bone Grafting
Bone grafting replaces missing jawbone tissue to support implants or correct defects. When bone grafting is needed, our bone grafting guide explains the process, timeline, and how it prepares you for implants.
When bone grafting is needed:
- Insufficient bone for implant placement
- Missing bone from tooth loss or disease
- Cleft palate repair
- Reconstruction after tumor removal
- Trauma reconstruction
Graft sources:
- Patient’s own bone (autogenous – most successful)
- Donated bone from tissue banks
- Synthetic bone substitutes
Steps of Oral Surgery: What to Expect
Understanding the surgical process helps you prepare appropriately.
Step 1: Consultation and Evaluation
Your dentist evaluates your condition and refers you to an oral surgeon if surgical treatment is recommended.
During consultation:
- Detailed examination of surgical area
- Imaging ordered (X-rays, CT scans, 3D imaging)
- Medical history reviewed
- Medications and allergies documented
- Surgical options discussed
- Realistic expectations established
Time: 30-60 minutes
Step 2: Surgical Planning
Advanced imaging is studied and surgical approach is planned in detail.
Planning includes:
- 3D surgical models created for complex cases
- Surgical approach determined
- Potential complications anticipated
- Anesthesia plan established
- Surgical time estimated
Step 3: Pre-operative Instructions
You receive written instructions preparing for surgery.
Key instructions:
- Nothing to eat or drink before surgery (fasting prevents aspiration)
- Medications to continue or stop
- When to arrive before scheduled time
- What to wear
- Arrange transportation (you cannot drive after anesthesia)
Step 4: Anesthesia Administration
Anesthesia is administered based on procedure complexity.
Anesthesia options:
- Local anesthesia alone (patient awake, numbed area)
- Local anesthesia with IV sedation (conscious sedation, drowsy)
- General anesthesia (unconscious, full surgical conditions)
Local anesthesia ensures:
- Complete numbness of surgical area
- No pain during procedure (you may feel pressure)
- Faster recovery than general anesthesia
Step 5: Surgical Procedure
The surgical procedure is performed using specialized techniques.
Procedure times vary:
- Simple extraction: 15-30 minutes
- Surgical extraction: 30-60 minutes
- Dental implant: 60-90 minutes
- Bone graft: 60-120 minutes
- Jaw surgery: 2-4 hours
During surgery:
- Surgical site prepared with antiseptic
- Bone or tissue removal as needed
- Implant placement or grafting performed
- Careful tissue handling to minimize trauma
- Bleeding controlled throughout
Step 6: Closure and Recovery Room
Surgical site is closed and you recover from anesthesia.
Closure process:
- Surgical site irrigated and cleaned
- Tissues sutured to close wound properly
- Gauze placed to control bleeding
- Discharge instructions reviewed
Recovery monitoring:
- Vital signs checked frequently
- Anesthesia wears off gradually
- Pain management provided as needed
- Transportation confirmed
Recovery After Oral Surgery
Recovery timeline and expectations vary by procedure complexity.
Immediate Recovery (First 24 Hours)
Expect:
- Numbness from anesthesia (several hours)
- Mild to moderate pain (controlled with medication)
- Swelling begins developing
- Possible bleeding or oozing
Pain management:
- Prescribed pain medication as directed
- Ice application (20 minutes on, 20 minutes off)
- Head elevation while resting
Avoid:
- Disturbing surgical site
- Using straws (suction dislodges blood clot)
- Smoking (interferes with healing)
- Strenuous activity
- Hot foods/drinks
Days 2-7: Early Recovery
Expect:
- Peak swelling at 48-72 hours (normal)
- Pain decreasing each day
- Slight bruising may appear
- Sutures remain in place
- Restricted diet continues
Care:
- Continue ice first 48-72 hours
- Switch to warm compress after 72 hours
- Continue pain management as needed
- Keep surgical area clean
- Take prescribed antibiotics
- Eat soft foods
- Get adequate rest
Contact surgeon if:
- Excessive bleeding (not controlled with pressure)
- Severe pain uncontrolled by medication
- Fever above 101°F
- Increasing swelling after 72 hours
- Signs of infection (redness, warmth, pus)
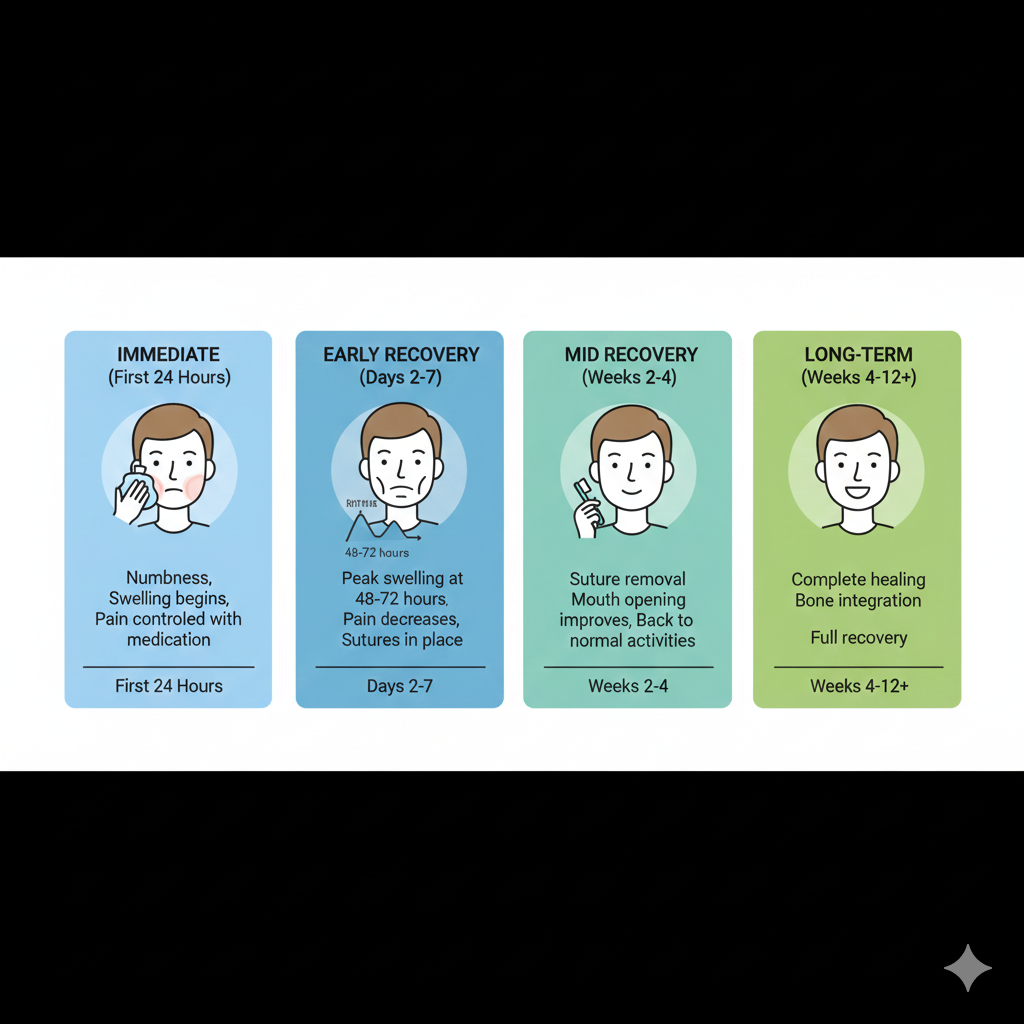
Weeks 2-4: Mid Recovery
Expect:
- Swelling mostly resolved
- Bruising fades
- Pain minimal
- Sutures removed (typically around day 7-10)
- Mouth opening improves
- Can return to most normal activities
Care:
- Careful oral hygiene (avoid surgical site)
- Suture removal appointment
- Gradually return to normal diet
- Resume normal activities gradually
Weeks 4-12+: Long-term Healing
Expect:
- Complete healing depends on procedure
- Bone healing continues (months)
- Full function restored
- Implants integrate with bone (3-6 months)
- Jaw surgery healing (6-12 weeks)
Benefits of Oral Surgery
Oral surgery provides significant benefits for appropriate cases.
Resolves problems – Addresses conditions that conservative dentistry cannot manage
Restores function – Improves ability to chew, swallow, and breathe properly
Improves appearance – Many procedures significantly enhance facial appearance and smile
Prevents complications – Removes problematic teeth before they cause abscess or bone loss
Long-term outcomes – Natural tooth replacement through implants lasts 20+ years
Risks and Complications
All surgery carries some risk. Understanding potential complications helps manage expectations.
Common minor complications:
- Swelling and bruising (normal, resolves in 7-14 days)
- Pain and discomfort (controlled with medication)
- Difficulty swallowing (temporary from swelling)
- Nausea from anesthesia (usually resolves within hours)
Uncommon complications:
- Excessive bleeding (rare in healthy patients)
- Infection (possible despite preventive measures)
- Dry socket after extraction (blood clot dislodges, causes pain)
- Temporary nerve numbness (usually resolves within weeks)
- Sinus communication (upper teeth near sinus, usually self-resolving)
Minimizing complications:
- Thoroughly disclose medical history
- Stop smoking before surgery
- Follow pre-operative instructions exactly
- Follow post-operative instructions carefully
- Avoid strenuous activity during healing
- Keep surgical area clean
- Take prescribed antibiotics
- Attend follow-up appointments
FAQ: Common Questions About Oral Surgery
Q: Is oral surgery painful?
A: Oral surgery itself is not painful because anesthesia completely numbs the surgical area. You may feel pressure and hear sounds, but not pain. Pain after surgery is normal and controlled with medication. Most pain is well-managed for the first few days, then decreases progressively.
Q: How long does recovery take?
A: Recovery timeline depends on procedure complexity. Swelling usually resolves within 7-14 days. Pain is minimal after 3-7 days. You can return to most normal activities within 1-2 weeks. Complete bone healing takes longer: 4-8 weeks after extraction, 3-6 months after implant placement, 6-12 weeks after jaw surgery.
Q: What should I eat after oral surgery?
A: Soft foods are essential for the first few days. Recommended foods include: yogurt, smoothies (avoid straws), applesauce, mashed potatoes, soup (warm not hot), pudding, cottage cheese, and scrambled eggs. Avoid hard, crunchy, spicy, or hot foods. Gradually progress to a normal diet as healing allows.
Q: When can I resume exercise?
A: Avoid strenuous exercise for 3-5 days after surgery. Light walking is acceptable the day after surgery. No heavy lifting, running, or intense workouts for 7-10 days. Return to exercise gradually as healing progresses. Increased blood pressure from exercise can cause bleeding.
Q: Can I smoke after oral surgery?
A: No, smoking should be avoided completely during healing. Smoking dramatically slows healing, increases infection risk, and increases dry socket risk. Tobacco chemicals interfere with blood flow needed for healing. If you smoke, quitting before surgery and staying quit during healing significantly improves outcomes.
Q: When should I call my surgeon?
A: Contact your surgeon immediately if you experience: excessive bleeding (not controlled after 30 minutes of pressure), severe pain unrelieved by medication, fever above 101°F, signs of infection (increasing swelling, redness, pus), difficulty breathing or swallowing, numbness extending beyond surgical area.
Q: What’s the difference between oral surgery and maxillofacial surgery?
A: Technically, oral surgeons are oral and maxillofacial surgeons (OMFS). The term reflects their training in treatment of both oral (mouth) and maxillofacial (upper jaw and face) regions. They treat conditions throughout this anatomical area. Some focus primarily on dental procedures; others focus on trauma and complex reconstruction.
Supporting Your Oral Health
Oral surgery is often necessary when conditions exceed conservative treatment options. Supporting your oral health before and after surgery optimizes outcomes.
Before surgery:
- Control medical conditions well
- Stop smoking (improves healing significantly)
- Complete necessary dental work
- Address infections before surgery
- Maintain excellent oral hygiene
After surgery:
- Follow post-operative instructions exactly
- Take prescribed medications as directed
- Maintain excellent oral hygiene
- Keep follow-up appointments
- Report any concerns immediately
Long-term care:
- Maintain excellent oral hygiene
- Regular professional cleanings
- Avoid smoking (dramatically reduces implant lifespan)
- Manage medical conditions well
- Early intervention for new problems
Final Thoughts
Oral surgery addresses conditions that cannot be managed with conservative dentistry, restoring function and oral health. Modern surgical techniques and anesthesia make procedures safer and more comfortable than ever before.
If your dentist recommends referral to an oral surgeon, it’s because specialized expertise will provide the best outcome for your specific situation. Understanding what to expect before, during, and after surgery helps you prepare appropriately and supports optimal healing.
Choosing a board-certified oral surgeon with appropriate training and experience for your specific procedure maximizes the likelihood of excellent outcomes and minimizes complications. Proper surgical intervention, combined with excellent post-operative care, provides long-term benefits that significantly improve your oral health and quality of life.