Teeth hurt when eating sweets because sugar reaches the sensitive dentin layer beneath your enamel the hard outer shell that protects each tooth. When enamel wears down, develops a cavity, or is compromised by a crack or gum recession, sugar gains direct access to thousands of microscopic tubules inside the dentin that connect straight to the tooth’s nerve, triggering a sudden sharp pain or “zinging” sensation. While a single episode of sweet sensitivity might not be serious, regular pain when eating candy, chocolate, or sugary drinks is your mouth signalling that something below the surface needs attention.
How sugar actually causes tooth pain the science explained
Your teeth are protected by enamel the hardest substance in the human body. Beneath the enamel sits dentin, a softer, porous layer filled with tiny fluid-filled channels called dentinal tubules. These tubules lead directly to the pulp, where the tooth’s nerve lives. When enamel is intact and healthy, it acts as a complete barrier between sugar and those nerve pathways. When it is not, the problem starts.
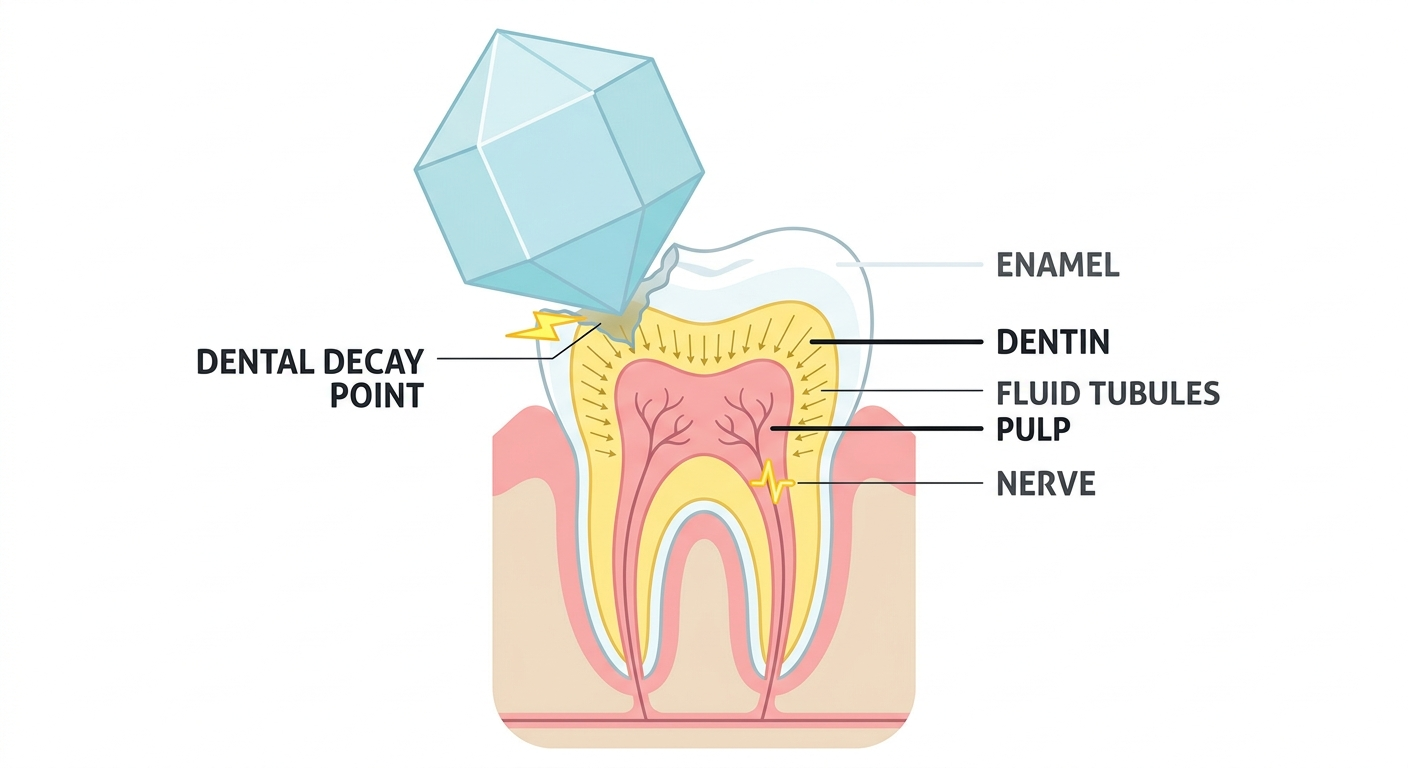
When you eat something sweet, the sugar does two things. First, it interacts directly with exposed dentin, drawing fluid through the dentinal tubules and triggering a nerve response this is what creates that sharp, sudden pain. Second, bacteria in your mouth feed on the sugar, producing acid as a byproduct. That acid attacks whatever remaining enamel is present, gradually widening the opening and making future sensitivity worse. This condition is medically known as dentin hypersensitivity, and it affects a significant number of adults at some point in their lives.
This is also why the pain from sweets can feel different from cold or heat sensitivity. Cold triggers a different fluid-movement response in the tubules. Sugar, however, creates an osmotic effect drawing fluid directly which is why it can cause a more immediate or intense reaction in people with moderate enamel loss, even when cold drinks cause no discomfort at all.
6 reasons your teeth hurt when you eat sweets
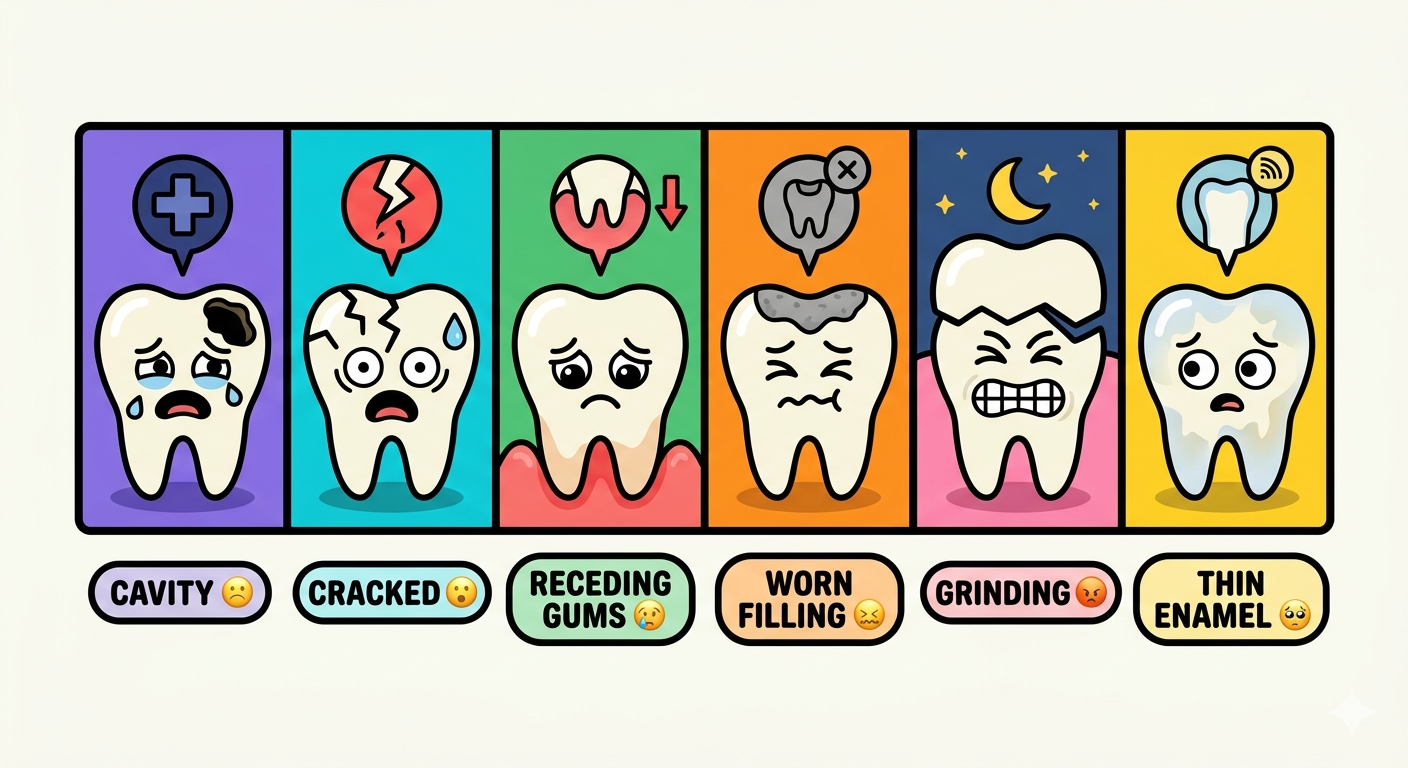
1. Enamel erosion the most common underlying cause
Enamel erosion is the gradual wearing away of the tooth’s outer protective layer. Once enamel is gone, it does not grow back making prevention the most important tool you have. Common causes of enamel erosion and tooth pain include drinking acidic beverages such as fizzy drinks, fruit juices, and sports drinks regularly; brushing too aggressively or using a hard-bristled toothbrush; frequent vomiting (as in acid reflux or eating disorders) which exposes teeth to stomach acid; and a diet high in sugar and refined carbohydrates over a long period.
As enamel thins, the dentin beneath it becomes progressively more exposed. At first, you may only notice sensitivity with very cold drinks or specific sweets. As erosion progresses, more foods trigger the response including things that were not a problem before. This gradual worsening is one of the clearest signs that enamel loss is the cause.
2. Cavities (tooth decay) when bacteria eat through your enamel
A cavity is a permanent hole in the tooth created by acid-producing bacteria. The process begins with plaque a sticky bacterial film that clings to the tooth surface. When you eat sugar, the bacteria in plaque convert it into acid within seconds. That acid demineralises the enamel, creating a soft spot that eventually becomes a hole. Once the cavity reaches the dentin layer, sweet foods trigger direct nerve pain every time they make contact with that spot.
A key sign that sweet sensitivity is caused by a cavity rather than general enamel wear is localisation the pain is concentrated in one specific tooth or area, rather than spread across multiple teeth. Early-stage cavities are often invisible to the naked eye, which is why regular check-ups are essential for detection before the pain stage. At Talpadent’s preventive dentistry service, routine examinations include cavity screening that can identify decay before it causes discomfort, avoiding the need for more complex treatment later.
3. Gum recession exposing unprotected tooth roots
Gums act as a protective seal around the base of each tooth. The tooth root, which sits beneath the gum line, has no enamel covering it is protected entirely by the gum tissue itself. When gums recede, those unprotected roots become exposed to everything in your mouth, including sugar. Because roots lack enamel, even small amounts of sugar coming into contact with them can trigger significant pain.
Gum recession develops gradually and is often painless until the exposure becomes significant. Common causes include gum disease (periodontitis), brushing too hard in a scrubbing motion, tobacco use, and genetics. If your sweet sensitivity is accompanied by teeth that look visually longer than they used to, or you can feel a notch at the gum line with your tongue, recession is a likely factor. Our periodontology service at Talpadent focuses on diagnosing and treating gum disease at the earliest stage, before recession causes lasting damage.
4. Cracked or damaged teeth
Teeth can develop hairline cracks that are invisible during a normal visual examination. These cracks create a pathway that allows sugar and bacteria to bypass the enamel surface and reach the dentin or pulp directly. The pain from a cracked tooth typically appears suddenly, is concentrated on one tooth, and may disappear quickly after the sweet is removed or it may linger.
Cracked teeth are caused by chewing hard foods, biting on ice, trauma to the jaw or face, or existing large fillings that have weakened the surrounding tooth structure. A dental crown is one of the most effective solutions for a cracked tooth it encases the entire visible portion of the tooth, preventing sugar and bacteria from accessing the crack and protecting the nerve from further irritation. Early treatment of a crack prevents it from deepening and ultimately reaching the pulp, which would require root canal treatment.
5. Worn or leaking dental fillings
Dental fillings do not last forever. Over years of chewing pressure, fillings can wear down, develop small cracks, or begin to pull away from the tooth wall leaving microscopic gaps between the filling material and the tooth. Sugar, bacteria, and saliva enter these gaps, reaching the dentin beneath and causing the same sharp sensitivity as an untreated cavity. If you have existing fillings and notice that one specific tooth has begun to hurt when eating sweets especially if the discomfort is new a worn or leaking filling is a likely cause. Replacing or repairing it promptly prevents the decay from progressing beneath the filling and reaching the nerve.
6. Teeth grinding (bruxism) a hidden cause many overlook
Bruxism the habitual grinding or clenching of teeth is one of the most overlooked causes of sweet sensitivity, and it is a content gap that most guides on this topic fail to address adequately. Teeth grinding most commonly occurs during sleep, making it difficult to detect without a dental examination. The repeated grinding motion places enormous pressure on the enamel, gradually wearing it flat and thin particularly on the biting surfaces and the sides of the back teeth.
As enamel thins from grinding, the dentin below becomes progressively more exposed, creating precisely the conditions that allow sugar to trigger nerve pain. The insidious aspect of bruxism-related sensitivity is that it worsens over time even without changes to diet because the enamel continues to wear down regardless of how carefully you eat. If you wake up with jaw soreness, headaches, or if your teeth look flatter and shorter than they once did, bruxism may be compounding any other sensitivity issues you are experiencing.
Why do sweets hurt my teeth but not cold or hot foods?
This is one of the most common questions dentists receive about tooth sensitivity, and it is almost never addressed in standard articles on this topic. The answer comes down to how different stimuli interact with dentinal tubules.
Cold temperatures trigger sensitivity through a rapid fluid shift in the tubule the quick change in temperature moves the fluid abruptly, which the nerve detects as pain. Sugar works through a different mechanism: osmosis. Sugar draws fluid out of the dentinal tubule rather than moving it with temperature. This osmotic pull stimulates the nerve via a different pathway, which is why some people are sensitive only to sweets, or more sensitive to sweets than to cold, depending on the specific location and extent of their dentin exposure. In practical terms, this means that sweet sensitivity and cold sensitivity are both signs of exposed dentin but they do not always appear together, and their absence in one form does not mean the other is fine.
Why do my back teeth hurt more when I eat sweets?
If the sweet sensitivity is concentrated in your molars or premolars rather than the front teeth, there is a specific anatomical reason. Back teeth bear the majority of chewing force every time you eat, your molars absorb significantly more pressure than your incisors. This greater mechanical stress means enamel wears faster on back teeth over time. Additionally, molars have deep grooves and fissures on their chewing surfaces that are natural traps for food particles and sugary residue. Sugar sits in these grooves longer than on flat surfaces, giving bacteria more time to produce acid and for the osmotic effect on dentinal tubules to occur. Back teeth are also more difficult to clean thoroughly, meaning plaque builds up in the grooves more easily accelerating both cavity formation and enamel erosion in that area.
What you can do at home to reduce sweet sensitivity
If the sensitivity is mild and has appeared recently, these measures can reduce discomfort and slow progression while you arrange a dental appointment:

- Switch to desensitising toothpaste products containing potassium nitrate or stannous fluoride help block the dentinal tubules over time. Use consistently for at least four weeks to assess the effect.
- Use a soft-bristled toothbrush and apply only light pressure. Aggressive brushing removes the protective gum margin and accelerates enamel wear.
- Rinse with water immediately after eating sweets this dilutes and removes sugar from the tooth surface before bacteria can convert it to acid.
- Wait 30 minutes before brushing after acidic or sugary foods the enamel is softened immediately after acid exposure, and brushing too soon causes additional wear.
- Eat cheese after sugary foods cheese raises the pH in the mouth and contains calcium and phosphate that help remineralise early enamel damage.
- Chew sugar-free gum containing xylitol stimulates saliva, which is the mouth’s natural defence system against acid. Sugar and oral health are directly linked through the role saliva plays in neutralising acids more saliva means faster acid clearance.
- Reduce frequency of sugary snacks it is not just the amount of sugar that matters but how often teeth are exposed to it. Five small sweet snacks throughout the day causes more damage than one dessert eaten in a single sitting.
Professional treatment options for sweet tooth sensitivity
Home care measures can reduce discomfort but rarely address the underlying cause. The appropriate professional treatment depends entirely on what is causing the sensitivity:
- Fluoride application in-office fluoride treatments are significantly more concentrated than anything available in toothpaste, and can remineralise early enamel damage and seal dentinal tubules in a single application.
- Dental bonding a tooth-coloured resin material can be applied over exposed dentin or root surfaces to provide a physical barrier between the sensitive area and sugar.
- Fillings if a cavity is the cause, a filling removes the decayed material and restores the tooth structure, eliminating the pathway sugar was using to reach the nerve.
- Crown placement for cracked teeth, severely worn enamel, or teeth with failing large fillings, a crown provides complete coverage of the exposed tooth, eliminating sweet sensitivity from that tooth entirely.
- Gum treatment if recession is causing root exposure, scaling and root planing or soft tissue procedures can address the underlying gum disease and, where possible, reposition gum tissue over exposed roots.
- Night guard for bruxism-related sensitivity, a custom-fitted night guard worn during sleep prevents grinding from further eroding the enamel surface.
- Root canal treatment in cases where sensitivity has progressed to the pulp and the nerve is involved, root canal treatment removes the infected or inflamed pulp tissue, eliminating pain at its source.
Accurate diagnosis is the key to selecting the right treatment. At Talpadent, we use advanced dental imaging including 2D digital X-rays and 3D Cone Beam CT scanning to identify cavities, cracks, and bone changes that cannot be seen during a visual examination, allowing us to design a precise treatment plan before any procedure begins.
Is it sensitivity or a cavity? How to tell the difference
| Sign | More likely: general sensitivity | More likely: cavity or deeper issue |
| Location of pain | Spread across multiple teeth or whole areas | Localised to one specific tooth |
| Duration of pain | Fades quickly after removing the sweet | Lingers or throbs after the sweet is gone |
| Triggers | Multiple triggers sweet, cold, hot | Primarily sweet or only one specific tooth |
| Onset | Gradual, worsening slowly over months | Sudden appearance or rapidly worsening |
| Visible signs | Teeth may look shorter or gums slightly lower | Dark spots, visible holes, or discolouration |
| Pain intensity | Sharp but brief resolves within seconds | Deeper, throbbing, or severe |
When should you see a dentist for sweet tooth sensitivity?
Sweet sensitivity that appears occasionally and resolves quickly may not require emergency attention. However, you should book an appointment at Talpadent as soon as possible if:
- The pain is concentrated on one specific tooth and does not fade quickly after the sweet is removed
- Sensitivity has appeared suddenly rather than developing gradually
- The sensitivity is getting worse week by week rather than staying stable
- You can see visible discolouration, dark spots, holes, or cracks on the affected tooth
- The pain has spread to include hot foods, cold drinks, or biting pressure not just sweets
- You are waking up with jaw soreness, headaches, or your teeth look noticeably flatter than before (bruxism signs)
- Over-the-counter desensitising toothpaste has made no improvement after four weeks of consistent use
At Talpadent in Steinfort and Limpertsberg, Luxembourg, Dr. Viorel Talpa and the clinical team treat tooth sensitivity from its root cause rather than masking the symptom. Whether the cause is a cavity, enamel erosion, gum recession, or bruxism, the right diagnosis leads to the right treatment and often a much simpler one than patients expect when caught early.

Frequently asked questions about teeth hurting when eating sweets
To reduce pain when eating sweets, switch to a desensitising toothpaste containing potassium nitrate or stannous fluoride and use it consistently for at least four weeks. Rinse with water immediately after eating sweets to remove sugar before bacteria convert it to acid. Avoid brushing for 30 minutes after eating sugary foods. These measures reduce discomfort but do not fix the underlying cause. If the sensitivity persists beyond four weeks or is getting worse, a dental appointment is needed to identify whether the cause is a cavity, enamel erosion, gum recession, or another condition requiring professional treatment.
Sudden sweet sensitivity as opposed to a gradual onset most commonly signals a new cavity, a cracked tooth, or a failing dental filling that has created a fresh opening for sugar to reach the dentin. It can also occur after teeth whitening treatments, which temporarily open dentinal tubules, making teeth more reactive to both sugar and cold. If the sensitivity appeared overnight or without an obvious cause, it should be assessed by a dentist promptly, as sudden changes in tooth sensitivity are more likely to indicate a specific structural problem than gradual sensitivity, which is more typical of slow enamel erosion.
The fastest home relief is to apply desensitising toothpaste directly to the sensitive tooth and leave it on without rinsing a thin layer applied with a fingertip before bed can reduce sensitivity more quickly than regular brushing use. Avoiding acidic drinks, very cold foods, and sweets for 24 to 48 hours also gives the dentin time to settle. For faster professional results, in-office fluoride treatments or dental bonding applied over the exposed area can provide near-immediate relief. However, these measures manage the symptom the only way to permanently eliminate sweet sensitivity is to identify and treat the underlying cause, whether that is a cavity, enamel erosion, or another issue.
The condition is medically known as dentin hypersensitivity or, more specifically in this context, sweet-triggered dentin hypersensitivity. It occurs when the dentin layer of a tooth is exposed and the dentinal tubules are open, allowing sugar to create an osmotic pull on the fluid inside those tubules, which stimulates the tooth's nerve and produces pain. Dentin hypersensitivity is a very common dental complaint and can be triggered by temperature, sweet foods, or touch, depending on which tubules are exposed and how open they are. It is not a diagnosis in itself it is a symptom that points to an underlying structural change in the tooth, which is why identifying and treating the root cause is essential.
Mild sensitivity that appears after starting a new whitening treatment typically resolves within one to two weeks as the dentinal tubules close again. Sensitivity from a new filling can also settle within a few weeks as the tooth adjusts. However, sensitivity caused by cavities, enamel erosion, gum recession, or cracks does not resolve on its own these are structural changes that can only worsen with time if left untreated. If sensitivity has not improved within two weeks of using desensitising toothpaste, or if it is worsening rather than improving, a dental appointment is the right step.
Yes, and there is a clear anatomical reason. Molars and premolars bear the majority of chewing force, meaning their enamel wears faster under mechanical stress. Their chewing surfaces also have deep grooves and fissures that trap food particles and sugar longer than the smooth surfaces of front teeth, giving bacteria more time to produce acid. These factors combine to make back teeth disproportionately vulnerable to both cavities and enamel erosion — which is why sweet sensitivity concentrated in the back of the mouth is very common. Regular professional cleaning of those deep grooves and prompt treatment of any fissure cavities is the most effective prevention.
Final thoughts
Tooth pain when eating sweets is almost never random it is your tooth communicating that something specific has changed. Whether the signal is coming from a thin patch of enamel, an early cavity, a gum line pulling back, a hairline crack, or a filling that has outlived its usefulness, the underlying cause is almost always treatable when it is found early. Waiting even if the pain is brief and manageable right now allows the problem to progress to a point where treatment becomes more complex, more time-consuming, and more costly.
The encouraging thing about most causes of sweet sensitivity is that they respond well to treatment at every stage. A fluoride application, a small filling, a crown, or a night guard can each eliminate the sensitivity entirely not mask it, but remove its cause. The challenge is identifying which solution applies to your specific situation, and that requires a clinical assessment rather than a self-diagnosis.
If sweets have started to hurt your teeth whether it is occasional discomfort or consistent sharp pain the team at Talpadent is here to find out why and give you a clear, straightforward plan to fix it. With clinics in Steinfort and Limpertsberg, Luxembourg, and advanced imaging technology to see exactly what is happening inside each tooth, we can move from assessment to treatment quickly, without guesswork.

Dr. Talpa is a licensed dentist with 12 years of clinical experience and owner of Advanced Smile Dental Care. Dedicated to making dental health information accessible, Dr. Talpa writes to help readers make informed decisions about their oral care. With a background in general and cosmetic dentistry, Dr. Talpa is passionate about translating complex dental topics into practical advice. When not treating patients, Dr. Talpa enjoys staying current with the latest advances in dental science and technology.